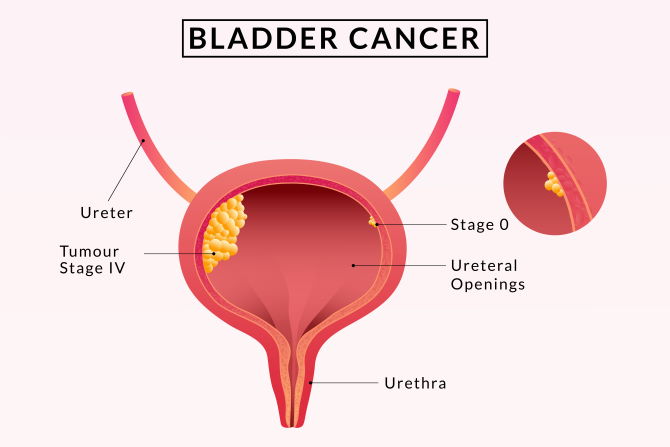
Bladder Cancer Symptoms and Treatments
Signs of bladder cancer include blood in your urine (haematuria), a burning sensation when passing urine, and needing to pass urine more frequently or urgently than normal. You may also experience pain in the lower abdomen or back area.
Depending on the extent of muscle-invasive cancer, surgery to remove your bladder may be recommended. Your physician might remove part (partial cystectomy) or all (radical cystectomy).
Chemotherapy
Chemotherapy drugs work to slow or stop cancer cells from growing and dividing, through oral administration or injection into veins (intravenous, or IV). They may also be administered directly into bladder tissue using catheters – sometimes in combination with radiation and surgery treatments.
Chemotherapy may be administered both prior to and following surgery. Preventative chemotherapy treatments known as neoadjuvant therapy can help ensure all cancerous cells are removed during a cystectomy procedure, potentially increasing its success rates.
Your doctor will decide how often chemotherapy treatments should take place; these could take place either at the hospital or as outpatient treatments. Blood tests will be done prior to each chemotherapy session to assess whether you can safely receive medicine and it may be wise for you to stop drinking fluids before treatments as this could dilute chemotherapy drugs in your system.
Your doctor may suggest intravesical chemotherapy using Bacillus Calmette-Guerin (BCG). Your healthcare team will administer an intravesical catheter which passes from your urethra directly into your bladder, then use this catheter to introduce BCG and chemotherapy drugs through it into the solution of your bladder for up to two hours before draining off and out of your body – usually as part of a day procedure in hospital.
If your risk of recurrence is higher, chemotherapy treatment may differ accordingly. One popular combination is Cisplatin combined with other drugs like Methotrexate, Vinblastine, and Doxorubicin; but every regimen will be tailored specifically for you.
Some chemotherapy medications may make you feel sick or tired and interfere with your appetite, leading to side effects like nausea and rash on the hands or feet, or sore throat. You can try minimizing their side effects by taking medication, eating healthily, and drinking plenty of fluids; if symptoms worsen contact your healthcare provider.
Radiation Therapy
If the cancer has not spread beyond your bladder, systemic drugs and radiation may be sufficient. If it has spread elsewhere, surgery, chemotherapy, or immunotherapy may be required; Mayo Clinic doctors can help find an approach that meets both your goals and needs.
Systemic chemotherapy treatments are drug treatments that work throughout your body to kill cancer cells and ease symptoms, as well as help prevent its return after other therapies have failed. You can take these medicines either intravenously (IV) or directly into your bladder; either alone or combined with radiation therapy – usually, combination drugs prove more successful than single ones; Examples include Cisplatin, Gemcitabine (Gemzar), Docetaxel (Taxotere) and Bleomycin (Bleomycin).
Radiation therapy uses beams of powerful energy such as X-rays or protons to destroy cancer cells. A doctor who specializes in providing radiation treatments to cancer patients is known as a radiation oncologist. You may require several sessions over days or weeks with their assistance – depending on how you feel during this period of time, depending on whether they want you working full-time or staying home during this period of treatment.
Immunotherapy may be an effective solution for advanced bladder cancer patients looking to prevent their cancer from coming back or spreading elsewhere in their bodies. Our immune systems contain cells designed specifically to combat infection and disease – including cancer! Using targeted therapies or biological agents as part of immunotherapy can stimulate your own immune system to fight back effectively against it.
Biological agents are compounds made of living organisms that help the body combat infections. Common biologic treatments used for bladder cancer include interleukin-2 (Ilutrix), adalimumab (Humira), and nivolumab (Bavencio).
An Immune Boosting Vaccine may also be given to increase your immunity and help protect you against bladder cancer, known as Bacillus Calmette-Guerin (BCG) vaccine. Doctors administer it by inserting a tube into your urethra, with follow-up appointments scheduled three or six months post-treatment until annual appointments become necessary.
Surgery
The bladder is part of your urinary system and responsible for producing and storing urine until you feel compelled to urinate, before discharging it through the ureters and urethra. Some individuals develop cancer that develops within cells lining their bladder – known as urothelial carcinoma – as well as cells lining the kidneys or upper urinary tract.
Your treatment options depend on the stage and extent of bladder cancer. A doctor will conduct tests to detect it as well as monitor its spread; such exams could include physical exams and pelvic exams, blood work analysis, imaging testing, urine collection samples, and CT scans of your abdomen and pelvis.
If your cancer is in its early stages (Ta, T1, or CIS) and hasn’t spread to the bladder muscle wall yet, surgery may be possible to remove the tumor while keeping your bladder functionally intact. You could also benefit from chemotherapy before or after surgery as well as radiation therapy.
Transurethral resection of bladder tumor (TURBT) involves inserting a thin and light tube through your belly button into your urethra in order to remove cancerous tissue. Your doctor might also administer the medication directly into your urethra that kills any cells left behind that may remain cancerous.
For advanced-stage or muscle-invasive bladder cancer, surgery to remove your entire bladder may be necessary, as well as chemotherapy before and/or after to prevent its return. Your doctor may also provide you with a vaccine called Bacillus Calmette-Guerin (BCG) to boost your immunity system and protect you from further disease progression.
Whenever your doctor decides to remove your bladder, a surgery called urinary diversion may be performed so you can still pass urine. There are three different forms of this surgery; one converts part of your intestine into an artificial peeing tube for passing pee; two create reservoirs to store urine; and three create new bladders from sections of the bowel. Urine must then be drained into an external bag several times daily.